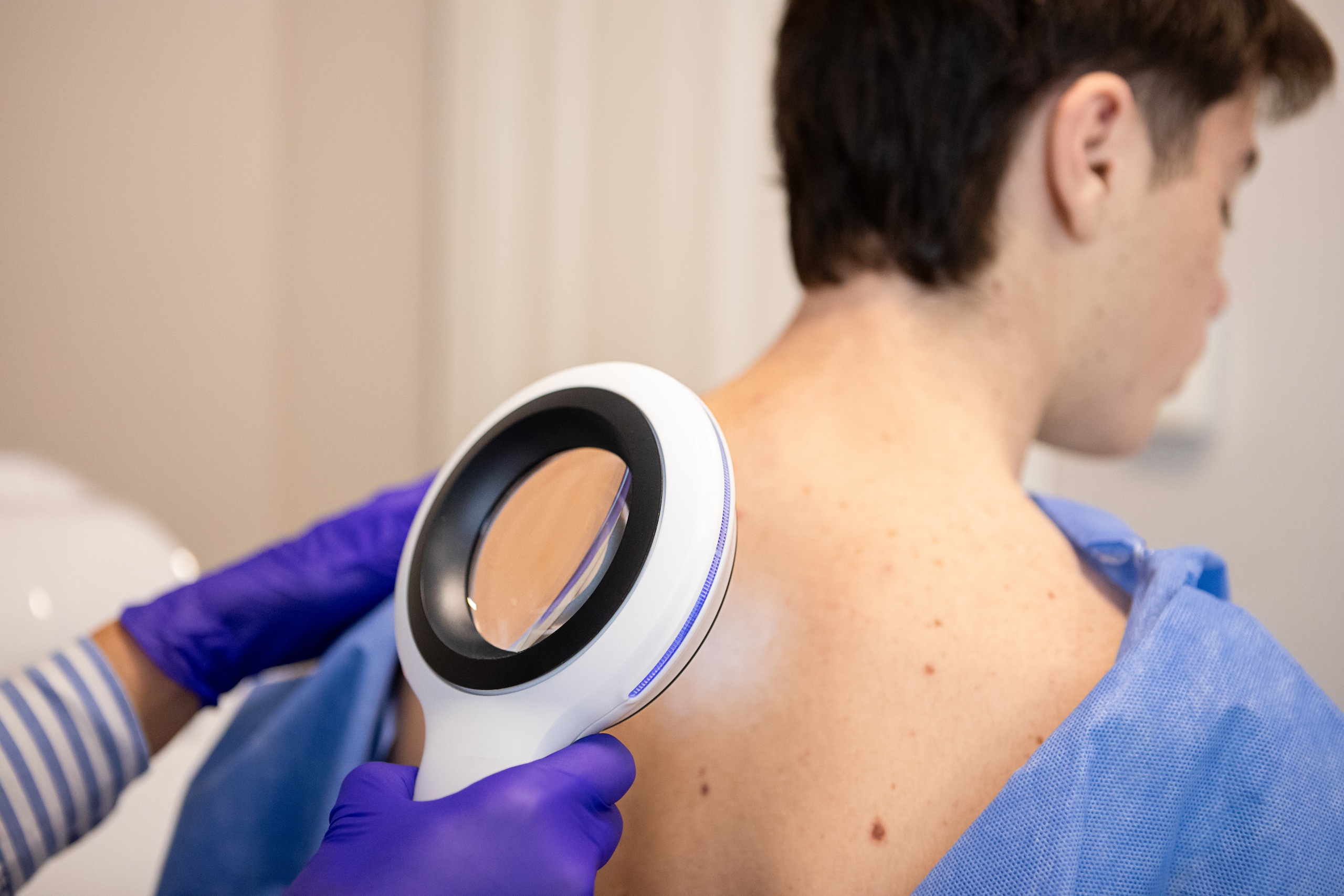
If you have melasma, a chronic condition that causes dark patches on your skin, it may affect how you feel about your appearance. And if it does, chances are that you’re open to anything you can do to reduce your melasma flare-ups.
Unfortunately, melasma is one of the most challenging skin conditions to manage for a number of reasons. But there is hope – recent research shows that you may have greater control over melasma than you think. The skin care experts at The Derm are here to explain the connection between alcohol consumption and other lifestyle factors that could be triggering your flare-ups.
What is melasma?
First, let’s take a closer look at melasma, including why it’s so difficult to manage.
Melasma is the medical term for patches of skin that are darker than your usual skin tone. This specific type of hyperpigmentation is very common and can happen to anyone. However, women with darker skin tones – and women in general – experience it far more often. According to the American Academy of Dermatology, women are 9X more likely to experience melasma than men during their lifetime.
Melasma often happens during a woman’s reproductive years, usually between 20 and 40 years of age. So it comes as no surprise that pregnant women frequently develop the condition. In fact, an estimated 15% to 50% of pregnant women will experience some form of melasma during their pregnancy.
Melasma can be caused by a wide range of factors, including:
-
- Sun exposure – Sun exposure is the biggest trigger for melasma, causing your skin to produce more melanin and form dark patches. Cosmetics and medications that make you sensitive to sunlight, such as antibiotics, retinoids, and nonsteroidal anti-inflammatory drugs (NSAIDs), may also contribute.
- Hormonal changes – Hormones like estrogen and progesterone, including the increased levels of these hormones during pregnancy, can also play a role.
- Genetics – Approximately 33% to 50% of people with melasma report that someone else in their family has it.
- Darker complexion – People with brown or black skin have more melanocytes (skin cells that produce melanin and darken your skin) than fair-skinned people.
- Skin care products – Any skin care products that irritate your skin can make melasma worse. (Ask your dermatologist about The Derm’s full line of professional skin care products.)
- Stress – Stress elevates your cortisol levels (a hormone that affects melanin production) and can worsen your melasma as well.
Melasma ranges from freckle-like spots to flat patches that are light brown, dark brown, or blue-gray in color. The most commonly affected area is your face (including your cheeks, nose, chin, upper lip, and/or forehead), but it can also appear on your arms, neck, chest, or back – any part of your skin that is exposed to sunlight.
Melasma typically darkens and lightens over time, worsening in the summer and then improving in the winter. Because it is a chronic condition, melasma can last for many years or your entire life. Other people may have melasma for just a short time, such as during pregnancy.
Why is melasma so hard to manage?
Melasma is especially hard to manage because it is deeply rooted in your skin and easily triggered by things like sun exposure, hormones, heat, and more. Melasma is harmless to you physically and does not hurt. However, it can have a major emotional impact, especially if you are embarrassed by how your skin looks.
Unfortunately, there is no treatment that can automatically make melasma disappear – and even after successful treatment, it may recur again and again. Therefore, researchers are now studying the connection between melasma triggers and lifestyle factors like alcohol consumption, smoking, caffeine intake, and more.
How alcohol might worsen melasma
A recent study published in Dermatology Times has confirmed that alcohol consumption can worsen melasma in multiple ways, including:
Oxidative stress
Alcohol induces oxidative stress, an imbalance where harmful free radicals overwhelm your skin’s antioxidant defenses, damaging cells and leading to inflammation (see below), hyperpigmentation, and other melasma-related concerns. Oxidative stress also accelerates the development of fine lines and wrinkles.
Redness and flushing
Alcohol dilates your blood vessels and makes your skin redder and more flushed, which can intensify melasma patches.
Dehydration
Moisture is an essential element in your skin’s defensive system. Alcohol is a diuretic, which means it can cause dehydration and dry out your skin, leaving it more vulnerable to melasma and other skin conditions.
Hormonal disruption
Alcohol consumption can also influence your estrogen levels, which is a known melasma trigger. Alcohol changes the way your body metabolizes estrogen, potentially increasing the amount of estrogen you produce.
Signs that your drinking habits might be affecting your melasma
Could alcohol consumption be making your melasma worse? Here are some signs to watch for:
-
- Your melasma darkens after social events, vacations, or other occasions where you consume alcohol more frequently
- You notice increased redness and/or flushing after consuming alcohol
- You have stubborn dark patches that aren’t responding to treatment
If alcohol consumption appears to be triggering your melasma, try drinking less alcohol – or if possible, cut alcohol out completely.
Treatment options for melasma
The Derm offers a variety of treatment options for melasma, based on the condition of your skin and your budget. In-office cosmetic treatment options may include:
-
- Chemical peels
- Laser therapy
- Microneedling
At-home treatment options and/or medications may include:
-
- Hydroquinone
- Azelaic acid
- Retinoids
- Tranexamic acid
- Vitamin C and other antioxidants
Protecting your skin from the sun and heat is a smart idea for anyone, but especially for people with melasma. Wear a broad-spectrum sunscreen with an SPF of 30 or higher every day, and avoid direct sun exposure, tanning beds, saunas, and other sources of intense heat. Even LED light from your television, laptop, phone, or other electronic devices can trigger a melasma flare-up, so expose your skin wisely.
When to see a dermatologist
If your melasma continues to worsen despite making lifestyle changes, the board-certified dermatologists at The Derm are here to help! To get started, schedule an appointment at our Glenview or Park Ridge office today.