Acne
*Individual Results May Vary
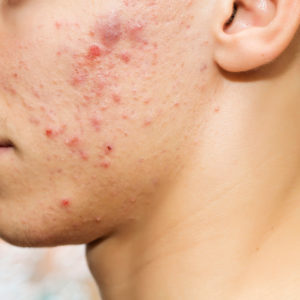
Acne is one of the most common diseases seen by dermatologists. It affects adolescents, as well as adults. Acne is a chronic disease and topical therapy may be required for the duration of the condition. It is likely to be interspersed with courses of oral antibiotics or other therapies, such as hormones (birth control pills, Spironolactone) or Isotretinoin.
Rosacea
*Individual Results May Vary
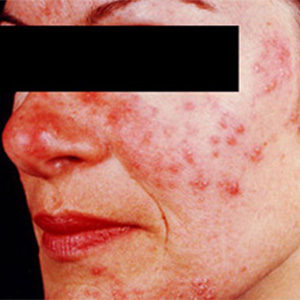
Rosacea is a common, but often misunderstood condition that is estimated to affect over 45 million people worldwide. It begins as erythema (flushing and redness) on the central face and across the cheeks, nose, or forehead, but can also less commonly affect the neck and chest.
Psoriasis
*Individual Results May Vary
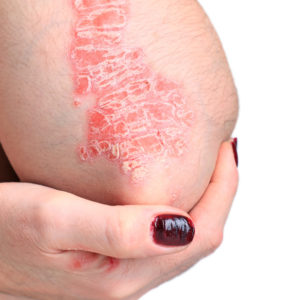
Psoriasis is believed to be an immune-mediated disease which affects the skin and joints. It commonly causes red scaly plaques to appear on the skin. The scaly patches caused by psoriasis, called psoriatic plaques or lesions, are areas of excessive skin production and inflammation. Skin rapidly accumulates at these sites and takes a silvery-white appearance. Plaques frequently occur on the skin of the elbows and knees, but can affect any area including the scalp, genitals and nails. Psoriasis is not contagious.
Melasma
*Individual Results May Vary
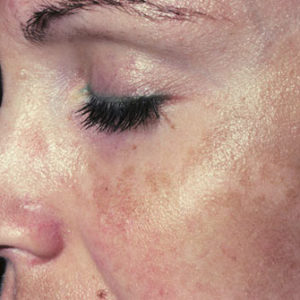
Melasma is a skin discoloration found on sun-exposed areas of the face. Melasma is a very common skin disorder. Though it can affect anyone, young women with darker skin tones are at greatest risk. Melasma is often associated with the female hormones, estrogen and progesterone. It is especially common in pregnant women, women who are taking oral contraceptives (“the pill”), and women taking hormone replacement therapy during menopause. Sun exposure is also a strong risk factor for melasma. It is particularly common in tropical climates.
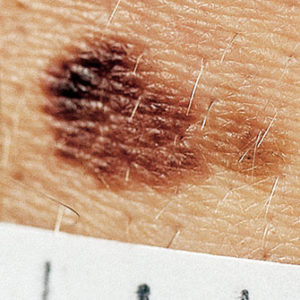
Skin Cancer Screening
*Individual Results May Vary
The physicians at The Derm encourage a yearly skin cancer screening for all of their patients. Skin cancer is the most common type of cancer in this country. About one million Americans develop skin cancer each year. There are many types of skin cancer. The two most common types are basal cell carcinoma and squamous cell carcinoma. These are sometimes called nonmelanoma skin cancer. These cancers usually form on the head, face, neck, hands, and arms.
Vitiligo

*Individual Results May Vary
Vitiligo occurs when the skin loses melanin, which is the pigment that determines skin, hair and eye color. This results when the cells that produce melanin are damaged or infected and no longer produce the pigment-forming material. It causes slowly enlarging white patches on the skin that may look like premature whitening or graying of the hair on the scalp, eyelashes, eyebrows or beard. The physicians at The Derm offer several treatment options, including phototherapy to treat vitiligo. Call The Derm and speak with a physician to discuss the best options for you.
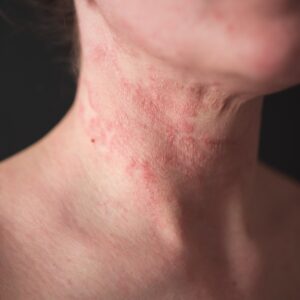
Eczema
*Individual Results May Vary
Atopic dermatitis, or Eczema, is thought to affect nearly 20% of children, even the youngest babies at times, and frequently develops during the first year of life. However, adults can develop atopic dermatitis at any time as well. Atopic Dermatitis is characterized by dry, scaly patches on the skin which can bubble up and then ooze and weep fluid; these patches are very common on the cheeks in infants. The condition is generally very itchy, and sometimes the itch is so intense that it is impossible to sleep.
Hair Loss Due To Skin Conditions

*Individual Results May Vary
Men and women of any age, even children, can experience hair loss, which can be caused by a variety of medical conditions such as thyroid problems, alopecia areata, scalp infections, hormonal factors, and as a part of other skin disorders. While daily shedding of hair is normal, if you start to notice that your hair is shedding in large amounts after combing or brushing, or if your hair becomes thinner or bald patches develop, you should consult one of the physicians at The Derm for proper diagnosis and treatment.
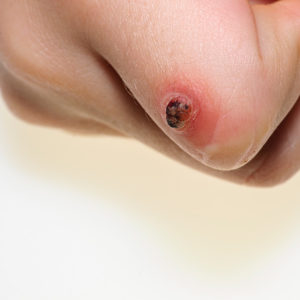
Warts
*Individual Results May Vary
Warts are common growths that are caused by the Human Papilloma Virus. This virus is present in the growths as well as on many surfaces touched by our hands and feet. Frequent touching and picking of warts may cause them to spread. Although some people may have a natural resistance to warts, it is advisable to avoid direct contact with warts on other people, and to wear foot protection such as sandals or rubber thongs in places where others go barefoot. Warts may develop on any part of the body including the face, scalp, lip, nose and genital area, as well as on the hands, feet, elbows, and knees.
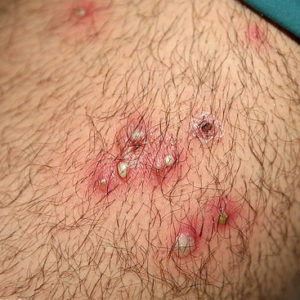
Folliculitis
*Individual Results May Vary
Folliculitis is an infection of the hair follicles in the skin. It is a common problem that is not usually serious. Tiny pus-filled spots (pustules) develop at the base of a hair, often in crops. Mild cases often resolve without treatment. Sometimes, antibiotic creams or tablets are needed. In recurrent cases, antiseptic skin washes can be used.
Skin Tags
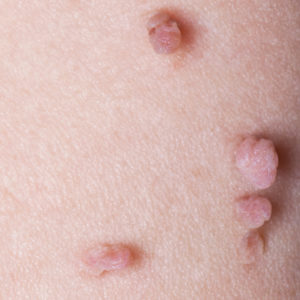
*Individual Results May Vary
Skin tags are usually more annoying to look at than anything else, but understanding what they are, and aren’t, can be reassuring. And though what causes skin tags isn’t always known, skin tag treatment is pretty straightforward — they are easily reduced.
Moles
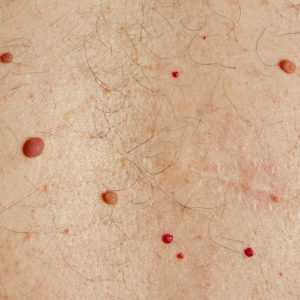
*Individual Results May Vary
A common mole is a growth on the skin that develops when pigment cells (melanocytes) grow in clusters. Most adults have between 10 and 40 common moles. These growths are usually found above the waist on areas exposed to the sun. They are seldom found on the scalp, breast, or buttocks
Shingles
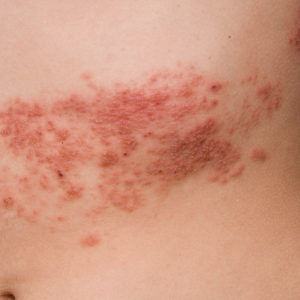
*Individual Results May Vary
Shingles is a viral infection that causes a painful rash. Although shingles can occur anywhere on your body, it most often appears as a single stripe of blisters that wraps around either the left or the right side of your torso.
Fungal Infections
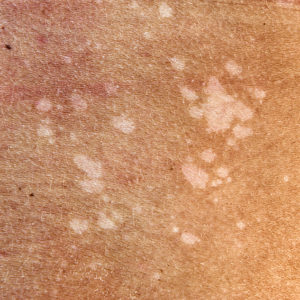
*Individual Results May Vary
Fungi usually make their homes in moist areas of the body where skin surfaces meet: between the toes, in the genital area, and under the breasts. Common fungal skin infections are caused by yeasts (such as Candida—see Candidiasis) or dermatophytes, such as Epidermophyton, Microsporum, and Trichophyton (see Overview of Dermatophytoses (Ringworm, Tinea)).
Chickenpox
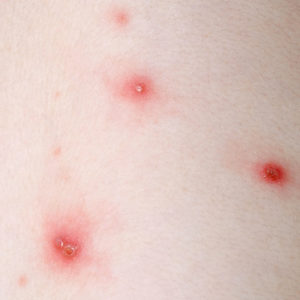
*Individual Results May Vary
Chickenpox used to be a common childhood illness in the United States, especially in kids under age 12. It’s much rarer now, thanks to the varicella vaccine that’s given when kids are between 12 and 15 months old, followed by a booster shot at 4 to 6 years of age.
